COPD Treatment Guide
Available treatment options
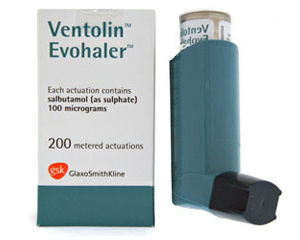
The foundation of COPD treatment is the use of bronchodilators —medicines that relax the muscles around your airways to open them up. For mild, occasional symptoms, I typically prescribe short-acting relievers like Ventolin , Salbutamol , or Bricanyl .
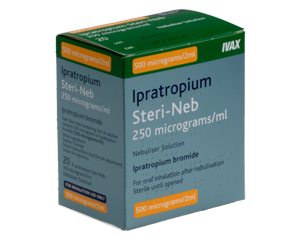
Another short-acting option is Atrovent , which works slightly differently to dry up secretions, or Ipratropium Steri-Neb for use in a nebuliser during severe flare-ups.
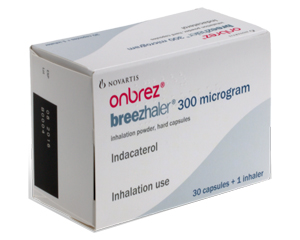
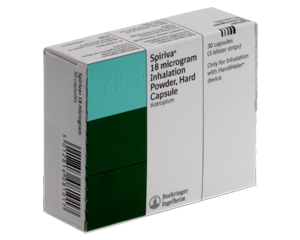
For daily maintenance, we move to long-acting inhalers. These are the real game-changers for quality of life. I frequently prescribe Long-Acting Muscarinic Antagonists (LAMAs) like Spiriva or Eklira , or Long-Acting Beta Agonists (LABAs) such as Serevent , Salmeterol , or Onbrez .
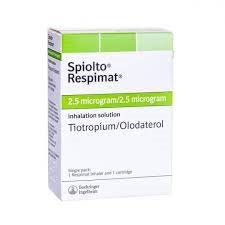
When one medication isn't enough, we use dual bronchodilators like Anoro or Spiolto to maximize airway opening.
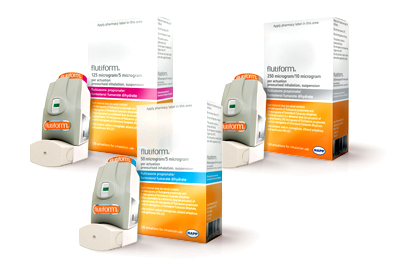
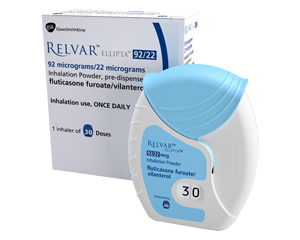
If you are prone to frequent chest infections, I will introduce inhaled corticosteroids to reduce inflammation. We usually use combination inhalers for this, such as Symbicort , Seretide , Relvar , or Flutiform .
Sometimes, standalone steroid inhalers like Flixotide or Pulmicort are used, though less commonly in COPD than in asthma. My first recommendation is always tailored to your specific symptoms, but a daily LAMA like Spiriva is often my starting point for newly diagnosed, symptomatic patients.
What to expect from treatment
A common pitfall I see in my practice is patients expecting their daily preventer inhaler to work like a magic wand. Here is a vital clinical insight: inhaled steroids and long-acting bronchodilators take time to reach their full therapeutic effect.
While a reliever works in minutes, your daily maintenance inhaler might take up to two to four weeks to noticeably reduce your breathlessness and mucus production. Please do not stop taking them just because you don't feel an immediate "hit." Consistency is the secret to preventing hospital admissions.
Self-care and prevention
Medication is only half the battle. Quitting smoking is the single most effective way to stop COPD from progressing—it is never too late, and I have seen lung function decline halt dramatically in patients who quit in their 60s and 70s.
Beyond that, keeping active is crucial. Finally, here is a practical tip for the UK winters: cold air triggers airway spasms. I advise my COPD patients to loosely wrap a scarf around their nose and mouth when stepping outside in December and January.
This creates a microclimate that warms and humidifies the air before it hits your sensitive lungs, preventing that sudden, tight-chested feeling.