Migraine Treatment and Prevention Guide
Available treatment options
We generally divide treatments into two categories: acute (taken when an attack starts) and preventative (taken daily to reduce frequency). For acute relief, the gold standard is the triptan family.
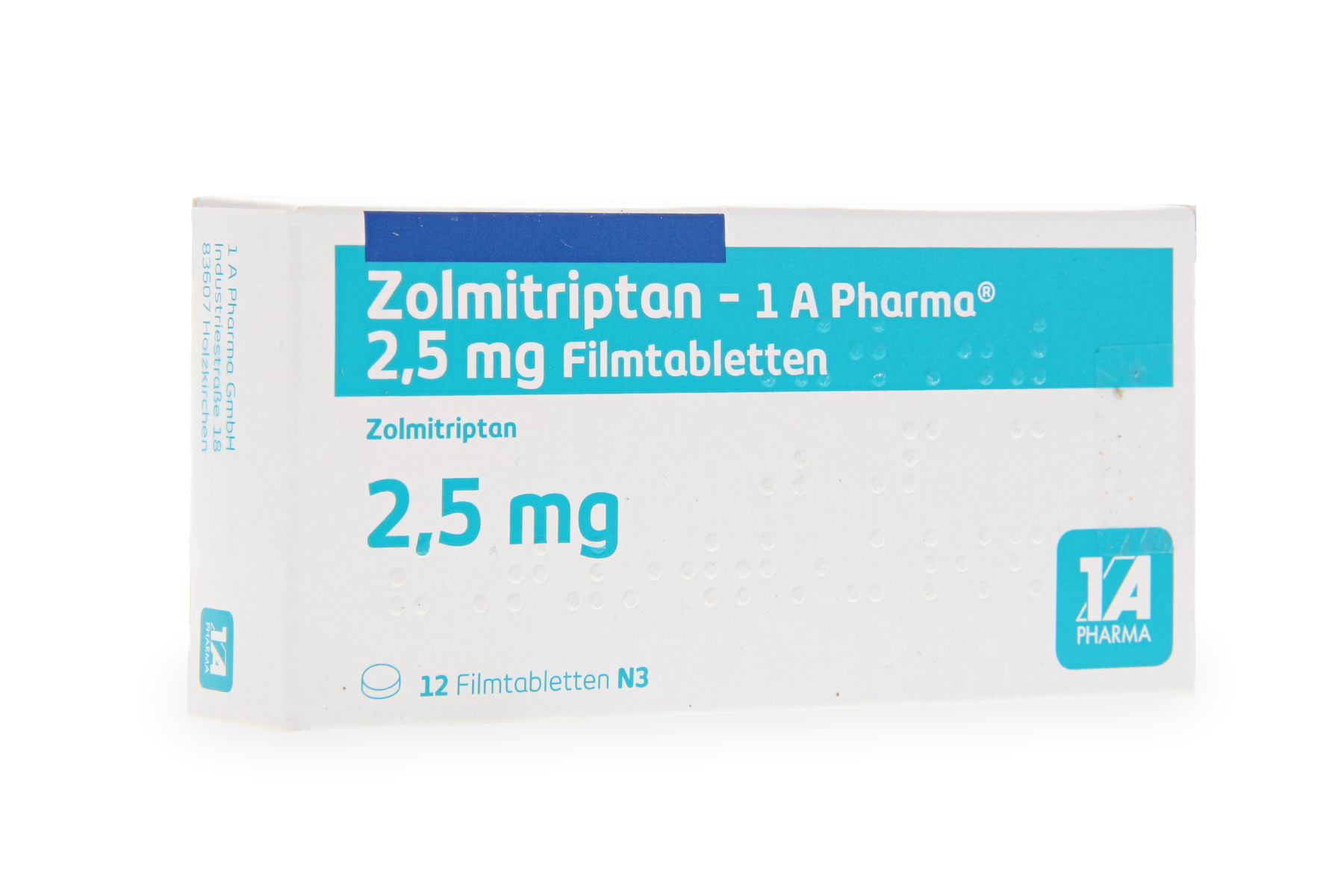
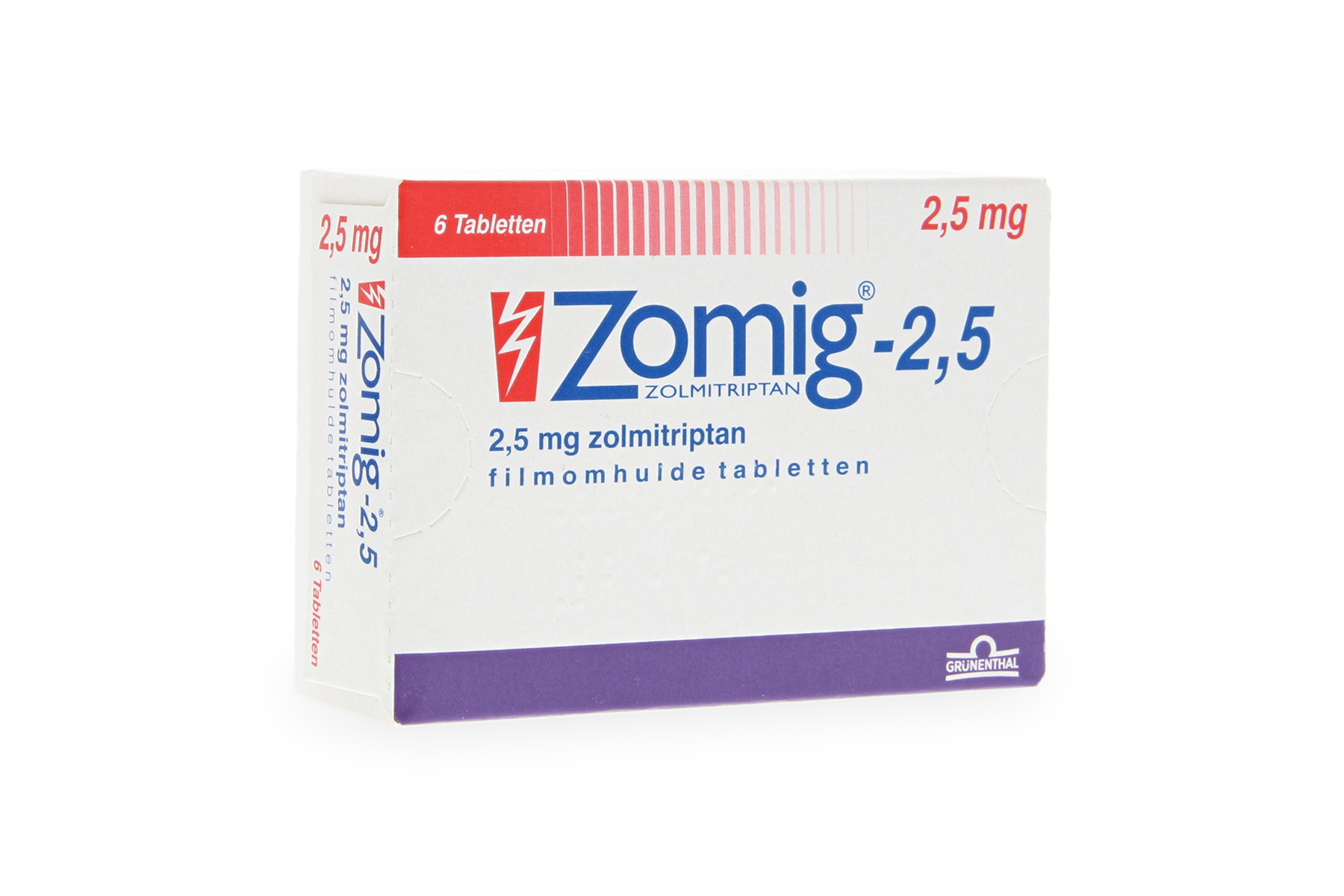
I often prescribe Sumatriptan as a first-line option, as it works quickly to constrict swollen blood vessels. If that causes too many side effects or isn't effective, we might try Rizatriptan (often known by the brand name Maxalt ) or Zolmitriptan ( Zomig ), which some patients find more tolerable.
For patients who have longer-lasting migraines, particularly those tied to the menstrual cycle, I frequently recommend Naratriptan ( Naramig ). My clinical pearl here is that while Naratriptan takes a bit longer to kick in, it stays in your system longer, making it excellent for preventing the "rebound" migraines that happen the next day.
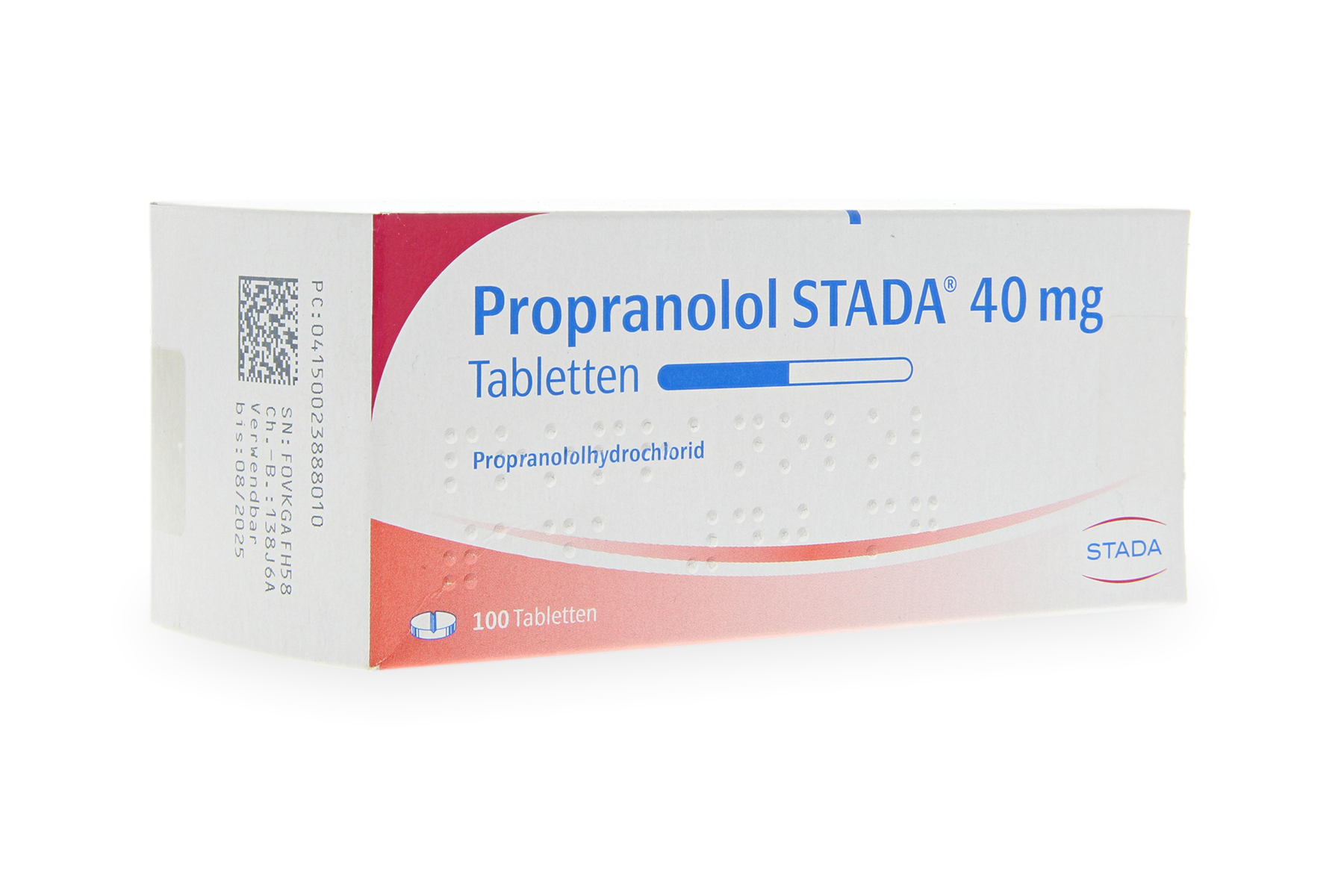
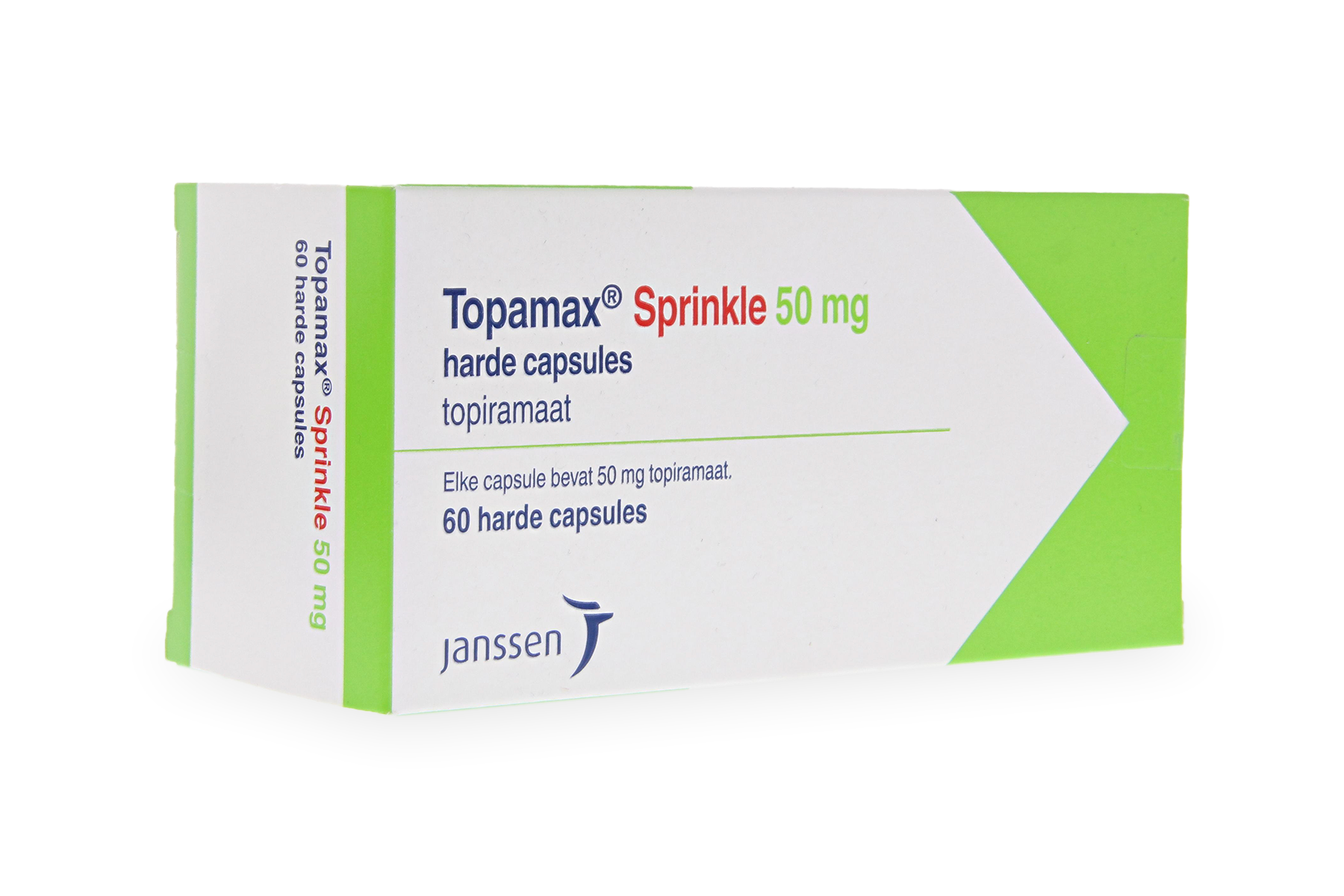
For prevention, we have several reliable options. Propranolol , a beta-blocker, is fantastic for patients who also experience anxiety or palpitations. Topamax (topiramate) is another highly effective preventative, though we must monitor for side effects like tingling in the fingers.
Occasionally, Clonidine is used for prevention, particularly in patients who also suffer from menopausal hot flushes, though it's less commonly my first choice nowadays.
What to expect from treatment
When taking a triptan, timing is everything. You must take it at the very first sign of the headache phase, not during the aura, and certainly not waiting until the pain is unbearable.
A common experience I warn my patients about is the "triptan sensation"—a feeling of heaviness, tingling, or slight tightness in the chest, neck, and throat. While this can feel alarming, it is usually a harmless side effect of the medication working on your blood vessels and typically passes within 30 minutes.
Preventative medications, on the other hand, require patience; they often take 6 to 8 weeks of daily use before you'll notice a significant reduction in your migraine days.
Self-care and prevention
Medication is only half the battle; your brain craves routine. While many patients know that dehydration, stress, and certain foods (like aged cheese or red wine) are triggers, the most overlooked trigger in my practice is inconsistent sleep.
My practical advice: wake up at the exact same time on weekends as you do on weekdays. "Sleeping in" on a Saturday alters your blood sugar and caffeine withdrawal timelines, which is why so many of my patients suffer from "weekend migraines." Maintaining a rigid sleep schedule is one of the most powerful, free preventative tools you have.